A client asked me the other day if I was to address a room full of GPs what would I say to them? For me this begs the question; is there something I would love medical practitioners and the public at large to understand about what we as manual therapy professionals do and why we do it that appears to not already be understood? Great question… here’s my answer.
Arthritis and degeneration in the spine, clinically known as spondylosis is NOT the real problem causing the pain in most of their client’s spines. Sure it can be a problem, it can be incredibly debilitating, painful and disabling but it is not the real culprit. It’s more of a symptom in fact, a CONSEQUENCE of long term unattended to, dare I say neglected, spinal dysfunction.
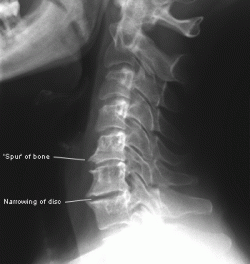
Case in point…the two most common regions in the human spine where we find premature spinal degenerative change is either in the lower neck or cervical spine (typically C5-7 as depicted in the attached picture) or the lower lumbar spine (L4-S1). The reason for this is that when you look up and down or turning your neck to change lanes when driving, your spine moves all the way from the top of your neck down to around the T4 or T5 thoracic vertebra which are located directly between your shoulder blades and functionally this constitutes your upper spine.
Now when we become tense around the upper shoulders from mental tension or poor posture, the upper thoracic spine (T1-T3) loses its mobility and tightens, making the lower part of the cervical compensate and move more to cover for what the T1-3 region is no longer doing. Over time this causes the lower cervical spine to become irritated, mechanically over-loaded and inflammation to build in the joints in this region of the spine. This is spinal arthritis! Artha = joint, itis = inflammation, so inflammation in a joint is the real meaning of the word arthritis. The thing is that this inflammation, if left unresolved and allowed to continue long term, (due to unresolved spinal mechanical dysfunction) leads to the eventual beginning of erosion of the joint surfaces, scar tissue formation within the joint capsule and boney remodelling or spur formation around the edges of the joint. All of which result in the eventual wear and tear and degenerative change we associate with the word arthritis.
So spinal degeneration is the consequence of unresolved dysfunction and mechanical over-loading of certain regions of the spine. The same occurs in the lower lumbar spine because it attaches to the pelvis and is also an inherently stiff structure which can stiffen more from excessive sitting or the repetitive movements associated with simply being left or right handed. Combined with tightness in the gluteal muscles and the sacro-iliac joints, this causes distortion and stiffness within the pelvis. This causes the tail bone (the sacrum) not to mesh nicely with the lowest lumbar vertebra (L5) and as a consequence, mechanical loads up this juncture. So you now have the situation where the lower lumbar spine (L4-5) is trying to do more, but it is doing it in an “out of alignment” environment. This does not make for very happy lower lumbar facet joints or intervertebral discs (the facet joints are at the back of the spine and guide the spines movements, the discs are at the front and are designed to move but also carry most of the weight bearing load). This situation is compounded by the fact that the lower thoracic spine or thoraco-lumbar junction (T10-L1) is another region which is prone to stiffness and dysfunction. This is due largely to the fact that most of the erector spinae muscles coming up from the pelvis that hold us up, attach here and as a consequence can cause this region to stiffen up and change in alignment as well.
So you can see how with years of gradual tightening in these regions due to stressors such as poor posture, muscle weakness or mental tension leads to both alignment and mobility changes that result in mechanical over-loading of these vulnerable regions within our lower cervical and lower lumbar spines. Left unchecked this can progress through a series of pathological changes that lead to the development of spinal arthritis or spinal degenerative change. A good reason to keep your spine functioning at its best…after all it’s the only one you’ve got! A final note is that these complaints are typically associated with weak core stability muscles which protect our spine and maintain good posture but that my friends will be the topic for my next article.